Complement System: Immunity’s Hidden Weapon
Before your body produces specific antibodies against a new invader, a powerful defense system is already hard at work. Meet the complement system— one of the immune system’s fastest and most sophisticated weapons. This ancient cascade of proteins can detect, tag, and destroy pathogens within minutes, while also bridging innate and adaptive immunity.
What Is the Complement System?
The complement system consists of more than 30 proteins circulating in your blood, tissue fluids, and on cell surfaces. Most exist in an inactive form until triggered by infection, antibodies, or abnormal cell surfaces. Once activated, they launch a precisely orchestrated cascade reaction that rapidly amplifies the immune response.
Think of it as a chain of dominoes: one small trigger sets off a powerful chain reaction with far-reaching effects.
The Three Key Functions of Complement
The complement system protects us in three major ways:
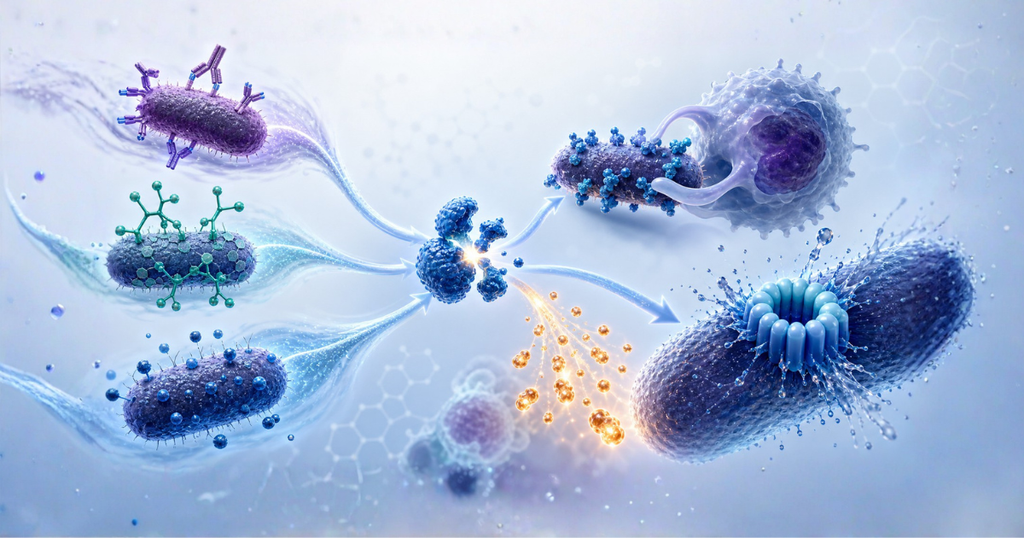
- Opsonization (Tagging for Destruction): Fragments like C3b coat the surface of bacteria, viruses, or damaged cells, marking them as “eat me” signals. This makes it much easier for phagocytes, such as macrophages and neutrophils, to recognize and engulf the targets.
- Inflammation and Cell Recruitment: Small fragments such as C3a and C5a, known as anaphylatoxins, act as powerful alarm signals. They increase blood vessel permeability, recruit immune cells to the site of infection or injury, and intensify local inflammation.
- Direct Cell Lysis: The terminal pathway assembles the Membrane Attack Complex, also called MAC or C5b-9, which punches holes in the membranes of target cells, especially bacteria, causing them to burst and die.
Complement also helps clear immune complexes, remove apoptotic, or dying, cells, and support adaptive immune responses, including B cell activation and antibody production.
The Three Activation Pathways
Complement can be activated via three distinct pathways that differ in their triggers but converge at a critical point: the cleavage of C3.
Figure 1: Schematic diagram of the three complement activation pathways, Classical, Lectin, and Alternative, converging at C3 and leading to the Membrane Attack Complex.
Brief overview of each pathway:
- Classical Pathway: Triggered primarily by antibodies, such as IgM or IgG, bound to antigens. The protein C1q recognizes these immune complexes and initiates the cascade. This pathway directly links the adaptive immune system to complement activation.
- Lectin Pathway: An antibody-independent route crucial in the early stages of infection. Mannose-binding lectin, or MBL, and ficolins recognize specific sugar patterns on microbial surfaces, activating associated proteases and leading to the same downstream effects as the classical pathway.
- Alternative Pathway: The most ancient and continuously active pathway. It begins with low-level spontaneous activation, or hydrolysis, of C3 and is strongly amplified on microbial surfaces that lack host regulatory proteins. This pathway acts as a surveillance system and serves as a powerful amplifier for the other two pathways.
All three pathways converge at C3, the central molecule of the complement cascade. C3 is cleaved into C3a, which is pro-inflammatory, and C3b, which acts as an opsonin. C3b then helps form C5 convertase, leading to C5 cleavage and ultimately the assembly of the destructive Membrane Attack Complex.
Tight Regulation: Preventing Friendly Fire
Complement is incredibly potent, so the body tightly controls it to avoid damaging healthy tissues. Human cells express multiple regulatory proteins, including:
- CD55/DAF and CD46/MCP: accelerate the decay of convertases and inactivate C3b.
- CD59/Protectin: prevents the final assembly of the MAC on host cell membranes.
- Factor H and Factor I: key fluid-phase regulators, especially of the alternative pathway.
These “brakes” ensure complement is fully activated only on foreign or damaged surfaces while being quickly shut down on healthy host cells.
When Complement Goes Wrong: Links to Disease
Dysregulation of the complement system contributes to many serious conditions:
- Complement deficiencies: Increase susceptibility to infections, especially with encapsulated bacteria like Neisseria meningitidis.
-
Overactivation or dysregulation: Strongly associated with:
- Paroxysmal nocturnal hemoglobinuria, or PNH
- Atypical hemolytic uremic syndrome, or aHUS
- C3 glomerulopathy and IgA nephropathy
- Age-related macular degeneration, or AMD
- Systemic lupus erythematosus, or SLE
- Certain autoimmune, inflammatory, and neurodegenerative diseases, such as Alzheimer’s disease
In cancer, complement can play complex and context-dependent roles.
Complement-Targeted Therapies: A Rapidly Growing Field
Complement has become a major therapeutic target. Several breakthrough drugs are already in clinical use:
- Eculizumab and Ravulizumab: Anti-C5 monoclonal antibodies used for PNH and aHUS. (Eculizumab Biosimilar)
- Pegcetacoplan: First C3 inhibitor, used for PNH and geographic atrophy in dry AMD.
- Iptacopan: Oral Factor B inhibitor targeting the alternative pathway, approved for PNH and under study for IgA nephropathy.
- Avacopan: C5a receptor antagonist used for ANCA-associated vasculitis.
Newer agents with improved delivery and specificity are expanding treatment options for kidney, eye, autoimmune, and inflammatory diseases.
Conclusion: An Ancient System with Modern Impact
The complement system is a masterpiece of evolutionary engineering— fast, powerful, and precisely regulated. It serves as a critical first line of defense while shaping the broader immune response. Understanding its mechanisms not only explains how we fight infections and maintain health, but also paves the way for innovative therapies for diseases once considered difficult to treat.
As research advances, complement-targeted therapies are poised to play an even greater role in modern medicine.
Have you ever encountered conditions related to the complement system, or are you curious about a specific pathway or therapy? Feel free to leave a comment below!
References
- Janeway’s Immunobiology
- StatPearls — Biochemistry, Complement
- Reviews in Frontiers in Immunology and recent pharmacological literature, 2024–2025